Ninetee years ago my son needed hemispherotomy as an infant (just three months old) to treat his seizures caused by hemimegalencephaly. My husband and I were desperate for seizure control and terrified of what surgery would mean for the rest of his life. Was such a drastic surgery really the treatment to pursue? It was an astoundingly difficult decision to make. The research was sparse and it was hard to know if we were doing the right thing.
Today, families facing similar decisions finally have something we did not: a comprehensive, evidence‑based guideline from the American Epilepsy Society (AES) that directly addresses treatment options for infants with epilepsy, including surgery. It was a great honor for me to be invited to serve on the guidelines panel and bring the voice of the families we serve to the guideline.
This guideline is written for doctors (clinicians) not parents. I’ll do my best here to interpret the guideline for you, but please remember that I am not a medical professional or researcher. I’m just a parent like you. Any questions you have about the guideline should be directed to your child’s medical team.
A note to doctors
If you’re a clinician reading this, please remember what an excruciating decision this is for a parent. It’s not going to feel like it fits in a tidy decision tree. You are asking parents to consider brain surgery for their child. This. Is. Huge.
Parents hear “surgery” and I promise you that they will feel fear, grief, and possibly relief all at once. They are trying to protect their child’s future from seizures and SUDEP, and also trying to protect their child from the risks of an operation on their brain. It is an awful place to stand. I remember feeling like I was slowly drowning in an open, dark sea when my husband and I were presented with this choice.
And parents have to make this decision while sleep‑deprived and often still reeling from the fact that their child even has epilepsy in the first place. So when you recommend a surgery evaluation, remember that you are shepherding a family through what for many is a traumatic experience. The neurosurgical terms that you use are confusing, so please answer the same question more than once if needed. Make it clear you’re not just handing them an option and walking away; stay with them through the process while they figure out what to do for their child.
Why this new guideline matters to us parents
This guideline is the first evidence‑based roadmap focused specifically on children age 1 month to 36-months old with epilepsy. It looks at three major treatment paths: medications, dietary therapies (like the ketogenic diet), and surgery. (The guideline does not include infantile spasms. Treatments for infantile spasms will be addressed in a separate guideline.)
For parents like us, this means:
-
There is now a structured way doctors are encouraged to think about treating your baby’s seizures, including when to stop “just trying another medicine” and start talking seriously about surgery or diet therapy.
-
The guideline highlights what drug-resistant epilepsy is: seizures that continue despite two appropriately chosen anti‑seizure medications used correctly.
-
Once a child has drug-resistant epilepsy, the guideline urges early referral to a specialized pediatric epilepsy center that has both surgical and dietary expertise, instead of waiting years in limbo (we’ve been shouting this from the rooftops for years).
In other words, if your baby’s seizures are not responding to anti-seizure medication, you’re not overreacting by asking about surgery. This guideline says those questions are appropriate and important.
Here’s the “decision tool” in the guideline (my notes highlighting some important points are in red):

The guideline is very clear that infants with drug‑resistant epilepsy with “structural lesions” (an area of the brain that looks different or damaged on a scan and can explain why seizures are happening) should be evaluated early – while trying the first medication – at epilepsy centers with expertise in this age group.
It also says that “(e)pilepsy surgery in infants and children 1 month to <36 months of age requires an experienced multidisciplinary pediatric team, including neurosurgery, epilepsy/neurology, anesthesia, neuroradiology, neuropsychology, neurocritical care, and nursing. For epilepsy surgery in infants and young children, ILAE Level 2 centers should be considered. This is particularly important for more extensive procedures such as hemispherectomies, hemispherotomies, or any epilepsy surgery in children <12 weeks of age.”
What is an ILAE Level 2 Center?
This is probably a topic for another blog post, but I’ll do my best to explain this here:
Most of us have heard about Level 3 and Level 4 epilepsy centers. These are hospitals that meet specific standards required by the National Association of Epilepsy Centers. They do not have pediatric-specific standards required of all these centers at this time. The International League Against Epilepsy (ILAE) is a global organization made up of epilepsy experts from many countries (in fact, the American Epilepsy Society is actually the north American chapter of the ILAE). The ILAE does many things, including reviewing the best available research and real‑world experience and then publish guidance on how epilepsy should be diagnosed and treated. When you see “ILAE” in a paper or guideline, think of it as a worldwide expert group trying to raise the standard of care everywhere.
In 2020, the ILAE published an important report called Establishing criteria for pediatric epilepsy surgery center levels of care: Report from the ILAE Pediatric Epilepsy Surgery Task Force. This report called for epilepsy centers to have two levels – level 1, for children age 9 and older, and level 2, for children age 8 and younger. The report recognized that young children, babies, and infants require a very experienced team. A few of the requirements for a Level 2 center include that the hospital must evaluate and treat at least 225 children with epilepsy each year, and perform at least 20 epilepsy surgeries per year (not including VNS implantation).
How the guideline talks about surgery
One of the most important parts of this guideline is that the strongest recommendations it makes are actually about surgery. There are many “conditional” recommendations (meaning the evidence is limited and families’ preferences matter a lot), but surgery for certain situations is different.
1. Hemispherectomy/hemispherotomy
The guideline makes a strong recommendation for hemispherectomy/hemispherotomy in infants and children with drug‑resistant epilepsy that affects one whole side of the brain (called “holohemispheric”), when it’s caused by specific problems like:
-
Sturge‑Weber syndrome
-
Perinatal stroke
-
Hemispheric cortical dysplasia.
For these children, the panel recommends hemispherotomy or hemispherectomy rather than continuing to add more medications.
Why such a strong recommendation?
There are lots of reasons the guideline gives a strong recommendation for surgery.
-
Drug‑resistant epilepsy in these conditions is considered life‑threatening, with a high risk of serious developmental harm and even death (including SUDEP) if left uncontrolled. A lifetime of drug-resistant seizures is dangerous. And seizures in infancy disrupt how the brain develops, which can prevent a child from reaching important milestones like walking, talking, and learning.
-
Surgery offers much higher chances of seizure freedom compared with trying different medications.
-
Studies reviewed in the guideline found that hemispherectomy/hemispherotomy can lead to seizure freedom in a majority of appropriately selected children, often in the range of 70-90 percent in otherwise very refractory epilepsy, though the evidence is still limited and comes from non‑randomized studies.
The guideline recognizes that this is not a easy decision for parents and is very honest that hemispheric surgery carries moderate risk, including immediate surgical risks and longer‑term risks like hydrocephalus, and the possibility that seizures could return over time. But when the alternative is relentless seizures damaging a developing brain, the balance tips toward surgery for many families.
2. Other resections and disconnections
For infants with drug‑resistant focal or lesional epilepsy (where the seizures come from one area or several areas, not the whole hemisphere), the guideline also makes a strong recommendation for:
-
Intralobar, multilobar, or focal resections
-
Posterior disconnections (like TPO – temporoparietaloccipital disconnection)
Again, these are recommended instead of continuing with medicines alone, because:
-
Drug-resistant epilepsy in this age group is considered life‑threatening if left untreated.
-
Surgery significantly increases the chance of seizure freedom or major seizure reduction, with acceptable complication rates at experienced centers.
The evidence for these surgeries is lower quality (mostly small studies), but taken together, they show that many infants who undergo resection or disconnection can achieve good seizure control and, in some cases, improved developmental scores.
3. Supratentorial Tumor‑related epilepsy
If a baby has seizures because of a brain tumor in the upper part of the brain, the guideline leans toward removing the tumor instead of not operating, but this advice is cautious because there are not many studies yet and the type and behavior of the tumor make a big difference in the decision.
4. Vagus Nerve Stimulation (VNS)
For vagus nerve stimulation (VNS), there is not enough published data in this specific age group for the guideline to make a recommendation one way or another. (The other day a parent shared that their child had VNS implanted at eight months old, so just because the guideline says there isn’t enough evidence, doesn’t mean that the surgery isn’t possible or won’t help.)
What “early surgery” really means for families
The guideline makes clear that the landscape of epilepsy surgery in children under 3 years of age has changed over the last three decades. This is because we now know more about two important truths:
-
Uncontrolled seizures in infancy can seriously harm cognitive and motor development.
-
When done in experienced centers, epilepsy surgery in infants can be safe and feasible and may improve both seizure control and developmental outcomes.
That means:
-
Not waiting “until they are older” if seizures are clearly uncontrolled and a structural lesion is visible on MRI.
-
Not endlessly cycling through medication after medication when the chance of them working is low.
-
Bringing in a whole team (epileptologists, neurosurgeons, anesthesiologists, neuroradiologists, neuropsychologists, and specialized nurses) to carefully evaluate the risks and benefits.
The guideline even notes that families place a huge emotional weight on surgical decisions and specifically calls out the need for compassionate communication and counseling throughout the process. That acknowledgment alone would have meant a lot to me 19 years ago.
Where medication and diet fit into the picture
Even though this post focuses on surgery, it helps to understand how surgery fits into the bigger treatment plan. You can read the guideline yourself to see what it says about medication and diet. However, the key takeaway is that the guideline says during surgical evaluation, a third medication can be trialed and/or ketogenic diet. It does not say to try a third medication first, wait until it doesn’t work, or try the ketogenic diet and wait to see if that doesn’t work. That would of course delay surgical evaluation – for our children, where time is of the essence, this is important.
Turning dense guidelines into questions you can ask
Clinical guidelines are written in technical language for doctors, but they are about your child’s life. Here are some concrete questions the AES guideline empowers you to ask:
-
“Does my child meet the criteria for drug‑resistant epilepsy?”
If your baby has tried two appropriate anti‑seizure medicines and is still having seizures, the answer may be yes, and that changes what should happen next. -
“Is there a structural cause on MRI that could make my baby a candidate for surgery?”
The guideline emphasizes early MRI and genetic testing to understand the cause of seizures. If there is a structural problem confined to one hemisphere or a focal region, surgery may be on the table sooner than you think. -
“Can we be referred now to a pediatric epilepsy center with surgical and dietary expertise?”
The document is explicit that children with persistent seizures should be referred to specialized centers, not managed indefinitely in general neurology without surgical input. -
“If surgery is an option, what type would you consider and what outcomes do you typically see?”
You can ask directly about:-
Hemispherectomy/hemispherotomy for hemispheric problems like hemimegalencephaly
-
Focal or multilobar resections or posterior disconnections for more localized lesions.
-
What I hope parents take away
If you are reading this because someone has mentioned epilepsy surgery for your infant, I want you to know:
-
You deserve clear, honest information about all options (medication, diet, and surgery) and how they fit together.
-
You deserve early referral to an experienced pediatric epilepsy center if seizures are not under control.
-
You deserve a team that sees you as a partner in decision‑making, not a bystander.
The AES infantile epilepsy guideline is not perfect, but it is a huge step forward. It tells doctors that surgery is not a last‑ditch option for “later,” but a potentially life‑saving, development‑protecting treatment that should be considered early.
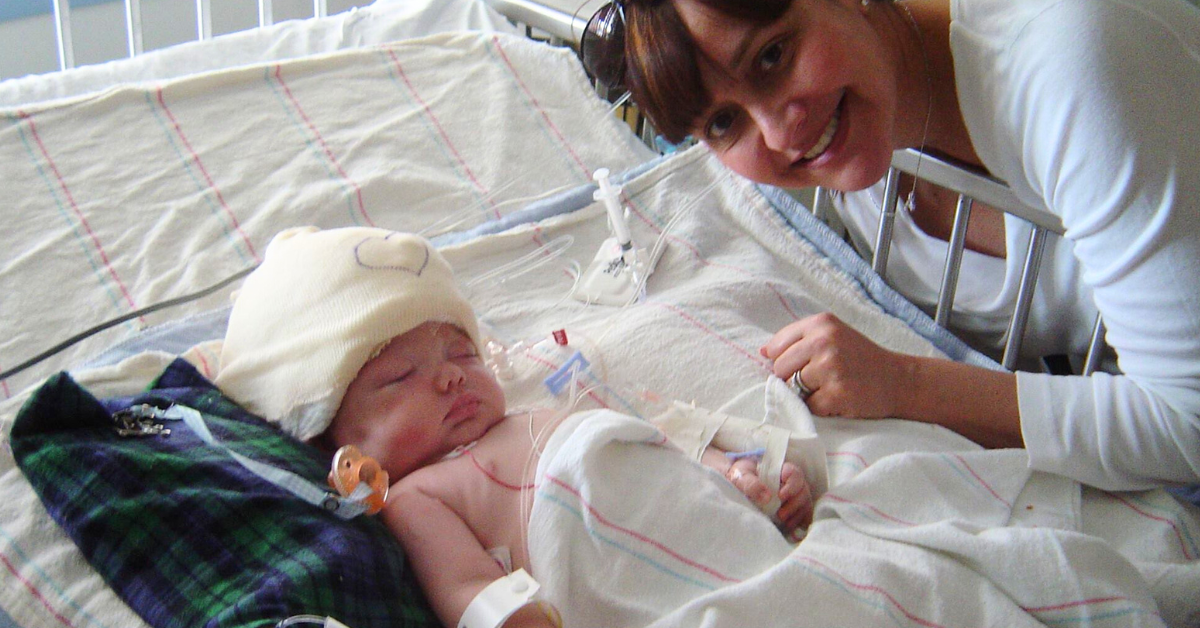
With my son, Henry, the day after his hemispherotomy.
about the author

Monika Jones, an inactive lawyer, is our founder and executive director. Her first son, Henry, had a modified lateral hemispherotomy, revision surgery, then true anatomical hemispherectomy to stop seizures caused by total hemimegalencephaly. She is also the principal investigator of the Global Pediatric Epilepsy Surgery Registry, the only parent-reported data collection to understand the developmental trajectory after pediatric epilepsy surgery. A strong believer in collaboration, she serves on the Pediatric Epilepsy Research Consortium‘s Research committee, the ILAE Neurobiology Commission’s Research Advocacy Task Force, and is an active member of the Rare Epilepsy Network and the Infantile Spasms Action Network. You can review her publications as well as contributions to collaborative research and advocacy projects at orcid.org/0000-0001-6086-3236.
Upcoming Events
Recent Posts
Stay Connected


